- Carbapenem-resistant Enterobacterales (CRE) infections are associated with increased morbidity and mortality, prolonged hospitalization, and limited treatment options. Their rising global prevalence makes CRE a significant public health concern.
- CRE resistance is most commonly mediated by carbapenemase enzymes (e.g., KPC, NDM, VIM, and OXA-48-like), which hydrolyze carbapenems and are frequently encoded on mobile genetic elements, enabling rapid horizontal spread.
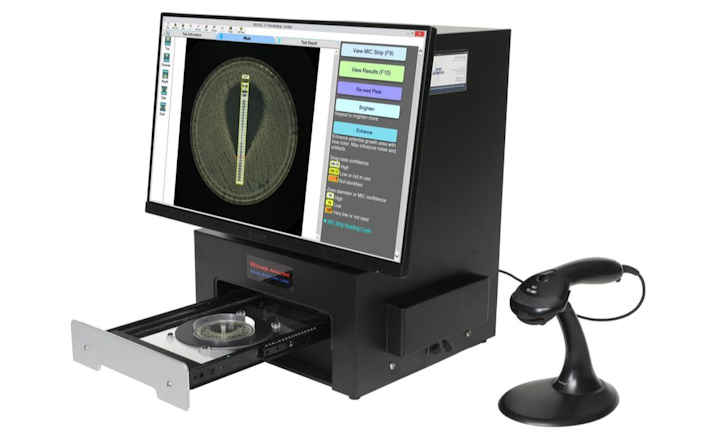
- Historically, clinical laboratories relied on MIC-only reporting to identify carbapenem resistance following revisions to CLSI breakpoints. Isolates exceeding susceptible carbapenem MIC thresholds were classified as CRE without routine determination of the resistance mechanism.
- The continued emergence of diverse carbapenemases, along with the availability of mechanism-specific therapies, has renewed the importance of carbapenemase detection. Updated CLSI guidance now recommends incorporating phenotypic and/or genotypic testing alongside MIC interpretation to support clinical management and surveillance.
Key Findings: Simner’s review summarizes the historical evolution of testing carbapenem-resistant Enterobacterales (CREs) and highlights several critical updates in CLSI M100 (2025).1
- Routine carbapenemase testing: The CLSI 2025 M100 update recommends routine carbapenemase testing using phenotypic and/or molecular methods to identify and differentiate enzymes such as KPC, NDM, VIM, IMP, and OXA-48-like, rather than relying on MIC-only reporting. Mechanism identification supports targeted antimicrobial therapy.
- Screening strategy considerations: Although ertapenem remains the most sensitive carbapenem for detecting carbapenemase production, screening strategies should be guided by local epidemiology, as resistance to ertapenem is now common in many regions.
- Types of carbapenemase tests: Carbapenemase detection methods can be broadly categorized into:
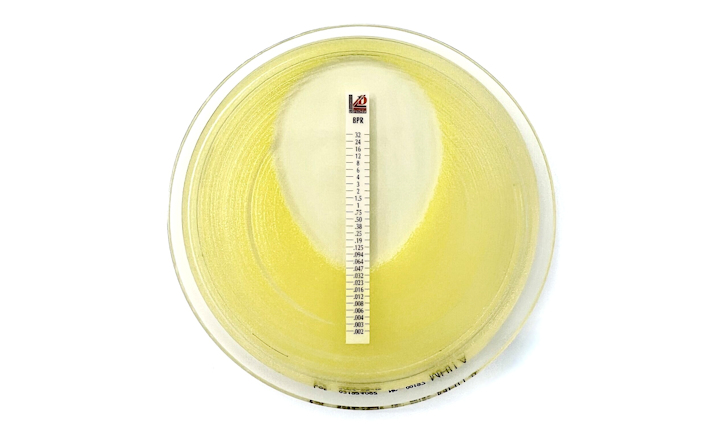
- Broad detection assays: e.g., Carba NP, modified carbapenem inactivation method [mCIM]), which distinguish carbapenemase-mediated resistance from non-carbapenemase mechanisms.
- Differentiation assays: including molecular (gene-based) and lateral flow immunoassays, are used to identify specific carbapenemase types. These assays typically target common carbapenemasez e.g. KPC, NDM, VIM, IMP, and OXA-48-like.
- Discrepancy resolution: provides structured guidance for resolving discrepancies between carbapenemase detection results and carbapenem susceptibility test results.
- Reporting recommendations: When carbapenemases are detected, CLSI recommends modifying susceptibility reporting (e.g., suppressing susceptible MIC interpretations for certain agents) to avoid misleading clinicians.
Bigger Picture: The updated CLSI guidance reflects a broader shift from phenotype-only susceptibility testing toward mechanism-based antimicrobial stewardship. While the MIC-only approach simplified workflows, it reduced visibility into resistance mechanisms that carry important therapeutic and infection control implications. Adoption of carbapenemase testing requires method validation, staff training, and workflow integration, but provides mechanism-based data that enhance therapeutic decisions, antimicrobial stewardship, and epidemiologic surveillance.
The renewed emphasis on carbapenemase detection aligns with the availability of mechanism-specific β-lactam/β-lactamase inhibitor therapies, where treatment success depends on identifying the underlying enzyme class. Resistance detection is therefore no longer purely epidemiologic—it is directly linked to therapeutic decision-making.
(Image Credit: iStock/ iLexx)