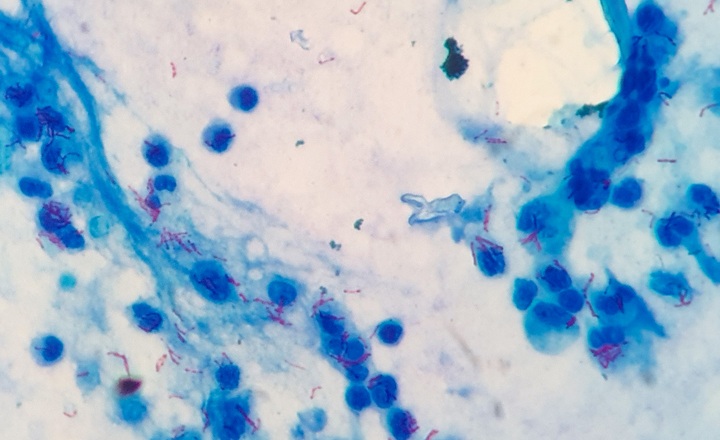
- Persistent diagnostic gaps in TB detection: Standard sputum-based testing remains difficult for key populations—including children, individuals with HIV, and patients with nonproductive cough—limiting case detection and delaying treatment.
- Non-invasive specimen types are operationally attractive: Saliva and oral swabs can be self-collected with minimal training, supporting decentralized testing strategies and community-based screening initiatives.
- WHO performance benchmarks drive assay development: The WHO defines ≥80% sensitivity as the threshold for low-complexity, non-sputum TB diagnostic tests, creating a quantitative target for alternative specimen validation.
Key Findings: This prospective, nested case–control study conducted by investigators from Colombia and collaborating U.S. institutions evaluated the diagnostic performance of molecular testing on paired saliva and oral swab samples using Xpert MTB/RIF Ultra.1
- Saliva demonstrated superior diagnostic sensitivity, exceeding WHO sensitivity targets for low-complexity non-sputum diagnostics:
- Sensitivity: 90.5% (95% CI: 82.8–95.6)
- Specificity: 95.8% (95% CI: 89.6–98.8)
- Meanwhile, oral swabs showed lower sensitivity but excellent specificity:
- Sensitivity: 71.6% (95% CI: 61.4–80.4)
- Specificity: 99% (95% CI: 94.3–100)
- High user acceptability supports real-world deployment: More than 95% of participants reported that saliva and swab collection procedures were acceptable, indicating strong feasibility for community-based implementation.
- Performance varied: Sensitivity of saliva testing exceeded the WHO 80% threshold for sensitivity among smear-positive individuals but declined among smear-negative and paucibacillary cases.
- Biomass input differences likely explain swab underperformance: Swab specimens contained significantly lower input volume (~0.1 mL) compared with saliva (~1 mL), resulting in lower total bacterial DNA input and reduced sensitivity.
Bigger Picture: This study by Vargas et al. indicates that saliva-based molecular testing is a viable alternative to sputum-based diagnostics for pulmonary tuberculosis, particularly in populations where sputum collection is impractical. Operationally, the performance of saliva testing supports expanded decentralized TB screening strategies, including home-based or community-based testing programs. While oral swabs offer logistical advantages, further optimization of biomass recovery and specimen processing will be necessary before they can reliably match saliva-based sensitivity in clinical diagnostics.
(Image Credit: iStock/ jarun011)