The World Health Organization (WHO) declared the Coronavirus Disease 2019 (COVID-19) outbreak, caused by severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2), a pandemic on March 11, 2020.1 Since then—at the time of writing—63,098,003 cases and 1,465,111 deaths have been reported from 191 afflicted countries/regions across the globe.2
Along with its high transmissibility and mortality (observed case-fatality ratio) rates, COVID-19 has elicited a universal psychosocial impact by bringing about mass hysteria, economic burdens, and financial losses.3 The resultant “coronaphobia,” or mass fear of COVID-19, has produced a variety of psychiatric manifestations that affect day-to-day life, including the management and prognostication of disease, relating to availability heuristics.
These cognitive biases have the potential to introduce prejudice that favors one outcome over another, playing a significant role in medical errors.4,5
In one particular study, 74% of diagnostic errors in internal medicine practice were linked to such cognitive factors.6 Reports like these underscore the importance of objectivity in healthcare; in the context of the COVID-19 pandemic, differential diagnosis is unequivocally paramount—especially in instances of co-infection.
During the 2009 influenza A(H1N1)2009pdm pandemic, reports of bacterial coinfection were plenty, resulting in substantially higher morbidity and mortality rates from misdiagnoses.7,11 The CDC estimated there were 60.8 million cases of H1N1 in the U.S, which, similarly, fostered availability biases.8
These cognitive factors precluded proper diagnosis of otherwise treatable bacterial and parasitic infections because they were mistakenly labelled as influenza.9 From a collection of 16 studies, bacterial coinfection rates for A(H1N1)2009pdm cases were 19% in ICU admissions and 12% in non-ICU admissions. Streptococcus pneumoniae was the culprit in 26% and 33% of ICU and non-ICU cases, respectively.
For those cases that didn’t present with bacterial coinfection at the time of A(H1N1)2009pdm diagnosis, nearly one in four patients developed a bacterial infection after the fact—a secondary bacterial infection. Prevention and treatment of these complications should thus be instituted as part of pandemic planning.7
Much like the 2009 influenza A(H1N1)2009pdm pandemic, clinicians have noted incidences of patients with COVID-19 that are experiencing coinfections. As such, many (early) studies report the empirical use of antibiotics for COVID-19 patients out of an abundance of caution—albeit inappropriate per antimicrobial stewardship.10,12
This dynamic has since shifted because there is now a paucity of data available that supports the routine use of antibiotics in the management of COVID-19 infection.11 Like other respiratory viruses, COVID-19 has a great degree of overlap with certain bacterial infections in symptomatology.12
While some hallmarks may be more characteristic of viral compared to bacterial infections (i.e. neutrophilic leukocytosis and lymphopenia, respectively), there is still a need for a quick differential diagnosis of potential respiratory pathogens when a patient presents with symptoms.
While nucleic acid tests are the gold standard for COVID-19 diagnostics, delays and reports of “false-negatives” are hampering timely diagnosis and treatment.13 As the demand for COVID-19 testing continues to rise, reference laboratories like LabCorp and Quest Diagnostics are reporting turnaround times for results of two to three days, respectively.14
While COVID-19 is certainly running rampant, the institution of secondary rapid tests may aid with differential diagnosis and prevent the oversight of complications that take the form of bacterial coinfection and secondary infection. Bacteria-based diseases like Legionnaires and pneumonia present symptoms that can be similar to those from COVID-19,15 but the treatments are different.
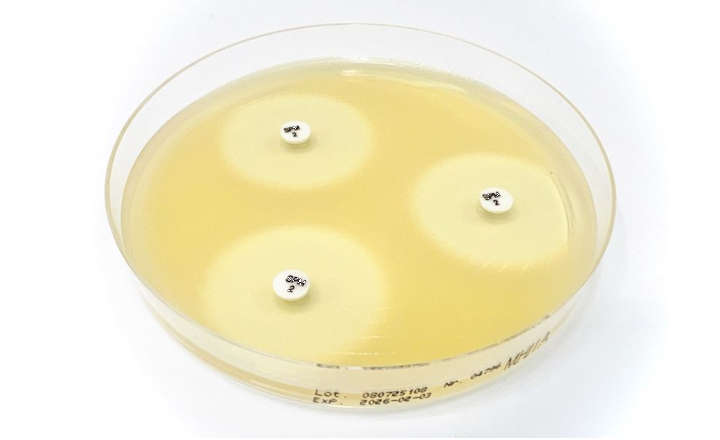
Simultaneous use of COVID-19 tests, as well as other tests, should be considered to ensure correct treatment. A rapid option is Immuview® S. pneumoniae & Legionella (P&L) Urinary Antigen Test as it allows professionals to quickly determine an appropriate course of action.
To further objectivity and stewardship in medical practice, Hardy Diagnostics has partnered with SSI Diagnostica to bring ImmuView P&L to its customers to aid in the differential diagnosis of bacterial pneumonia. This rapid assay produces results in 15 minutes and needs no equipment.
Authors:
Andrew Kravariotis – Business Development Manager, Hardy Diagnostics
Andre Hsiung – Chief Scientific Officer, Hardy Diagnostics
References:
- WHO: Rolling updates on coronavirus disease
- John Hopkins COVID-19 Dashboard by the Centre for Systems Science and Engineering
- Psychosocial impact of COVID-19
- The 'availability' bias: underappreciated but with major complications
- Cognitive Bias in the COVID-19 Pandemic
- Diagnostic error in internal medicine
- The role of pneumonia and secondary bacterial infection in fatal and serious outcomes of pandemic influenza a(H1N1)pdm09
- 2009 H1N1 Pandemic (H1N1pdm09 virus)
- A/H1N1 flu pandemic. Life threatening infections labelled swine flu
- COVID-19 Real-time learning network
- Co-infections in people with COVID-19: a systematic review and meta-analysis
- Recognition and management of respiratory co-infection and secondary bacterial pneumonia in patients with COVID-19
- Differential diagnosis of coronavirus disease 2019 from community-acquired-pneumonia by computed tomography scan and follow-up
- The demand for COVID-19 testing is up, stressing labs and delaying results
- COVID-19 rapid guideline: antibiotics for pneumonia in adults in hospital