Key Points
- Obligate anaerobe
- Commonest identifiable cause of antibiotic associated diarrhea
- Toxins A & B can cause illness independantly
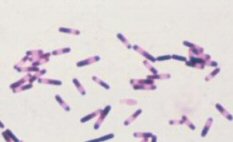
Recently, outbreaks of Clostridium difficile Associated Diarrhea (CDAD) have made the news headlines. C. difficile is the commonest identifiable cause of antibiotic associated diarrhea (AAD).
Following changes in the gut flora associated with the administration of broad spectrum antibiotics, the colon becomes colonised with this opportunistic organism which can produce two toxins: A and B.
Toxin A is an enterotoxin that causes fluid secretion, mucosal damage and internal inflammation. Toxin B is a more potent cytotoxin than toxin A, but is not enterotoxic. The toxins cause a characteristic mucosal damage consisting of plaque-like lesions that may lead to the formation of a pseudomembrane and pseudo-membranous colitis, severe cases may be fatal. Not all strains of C. difficile produce both toxins and some are not toxigenic at all and therefore do not cause any illness.
The discovery of C. diff strains (initially in North America and subsequently Europe) that have increased virulence has emphasised the need for effective screening and control measures.
Detection Techniques
Isolation of Clostridium difficile from stool samples is not diagnostic of CDAD but is important for the epidemiological typing of strains. Isolation is best performed after alcohol shock treatment. Stool samples are treated with an equal volume of methylated spirit or absolute alcohol, homogenised using a vortex mixer and left at room temperature for 1 hour, then inoculated on to Clostridium difficile selective agars e.g. CDSA with 7% horse blood; Cycloserine, Cefoxitin, egg yolk agar (CCEY), and incubated anaerobically for 40 - 48hrs.
Following primary selective culture, rapid latex agglutination tests allow identification of presumptive colonies of C. difficile within minutes. The latex particles are coated with antibodies specific for C. difficile somatic antigen. These screening tests can be used to reduce the number of samples that need to be progressed onto a toxin assay. If required confirmation may be done by biochemical identification tests.
For diagnosis of CDAD it is necessary to demonstrate the presence of C. difficile toxins. Toxin B may be detected by the production of a cytopathic effect (CPE) of faecal extracts on Vero cell cultures that is neutralised by C. sordellii antitoxin. It takes between 24 and 48 hours for a final result to be obtained. A CPE that is not neutralised by C. sordellii antitoxin may indicate that another pathogen is present in the faeces e.g. C. perfringens or Vero-toxic E. coli. Many labs use locally developed assays but commercial cytotoxity kits are available..
Direct testing of stool sample extracts for toxin presence using a variety of immunoassay techniques has largely replaced the culture method. The toxin is unstable at room temperature so the sample needs to be processed quickly or held refrigerated. Both toxins of C. difficile may be detected by these tests and there are a range of commercially available kits in different formats. As strains which only produce either toxin A or B have been reported as pathogenic, methods which detect both are preferable. For the high volume laboratory, microtitre plate or automated methods are available.
Assays can also be presented in a lateral flow format as single tests which give faster results, normally within a few minutes and with less operator skill requirements. Some assays are designed to detect C. difficile common antigen (glutamate dehydrogenase or GDH) produced by both toxigenic and non-toxigenic strains, and can also have a toxin test included in the panel so both toxin and organism may be revealed.
Studies using molecular detection of toxin A and B genes have been performed but they remain technically more demanding and hence more expensive and do not confirm expression of toxin. They do however allow identification of hypervirulent strains of C. difficile e.g. PCR ribotype 027 [or NAP1 in North Americas].
Comment
C. difficile infections are mainly healthcare associated, however there are increasing reports of community acquired infections. The need for the implementation effective infection control measures is clear.
Hypervirulent strains are of increasing concern.
The need for epidemilogical and antibiotic resistance data would appear to encourage a return to cultural techniques - at least in some targeted clinical situations.
Proficiency Testing
Clostridioides difficile proficiency testing can be part of a general Gastro Intestinal proficiency program and will assess the competency and accuracy of laboratories in detecting and identifying C. difficile infections.
Proficiency testing involves sending samples containing C. difficile or its toxins to participating laboratories. These samples are typically prepared by external proficiency testing providers or regulatory agencies. The laboratories then perform the necessary tests to identify the presence of C. difficile and determine its toxigenicity. The results obtained by the laboratories are compared to established standards or the expected outcomes, and their performance is evaluated.
Proficiency testing for C. difficile help assess laboratory performance, ensuring quality and accuracy of results, regulatory compliance and working towards continuous laboratory technique improvement.