Article by Yvonne Adebola (MSc, AMRSB), Global Health, Life Sciences and Technology Specialist
In South Africa, an outbreak of Listeriosis monocytogenes erupted leading to the worst listeriosis outbreak ever recorded in human history. On the 5th December 2017 an outbreak was officially declared by Dr Aaron Motsoaledi, South African Minister of Health. A total of 1060 cases of listeriosis were confirmed in laboratory tests between 1st January 2017 to 17th June 2018 reported to the National Institute for Communicable Diseases (NICD), the national public health institute of South Africa. This is compared to an average of 60-80 cases per annum reported in previous years.
The outbreak was first identified by medical doctors in July 2017 who notified the NICD of an abnormally high number of neonatal infections. The main provinces affected by the outbreak in South Africa included Gauteng, Western Cape and KwaZulu Natal which totalled approximately 80% of cases with the rest coming from other provinces. At least 200 people have been confirmed dead with hundreds more sickened. The most affected age group was neonates, followed by adults between 15-49 years of age.
Source of the Outbreak
Whole genome sequencing was performed on over 500 isolates to identify the strains with 91% of strains belonging to L. monocytogenes Sequence Type 6 (ST6). The ST6 sequence type was identified in a ready-to-eat processed meat product called “Polony” distributed by Tiger Brands Enterprise Foods. The source of the outbreak was identified as at Tiger Band’s Enterprise Foods’ Polokwane production facility and an official product recall was issued on 4th March 2018, though a voluntary recall was initiated by the company on February 14th following the detection of listeria from their own testing. Tiger Band’s Enterprise Foods along with three of its retailers’ export food products to 15 different countries across the African region, hence subsequent product calls were also issued.
During surveillance testing initiated by NCID other strains of L. monocytogenes were uncovered in facilities of different food manufacturers across the country leading to other food product recalls. This coupled with the minor percentage of non-ST6 strains found in infected patients may indicate that possibly more than one outbreak was occurring.
Between 19th-21st April 2018 a WHO Listeriosis Regional Technical Meeting occurred in Johannesburg with delegates from the Southern African Development Community across 16 countries to increase regional awareness of listeriosis as well as share knowledge and experiences. The meeting also served to steer countries to be able to respond and control listeriosis through contingency planning.
In early September 2018, Health Minister Aaron Motsoaledi announced that the outbreak was over as no new cases had been detected in the last 3 months. Following this, ready-to-eat processed meats were announced to be safe to consume however consumers are urged to ensure they practice proper food safety. Motsoaledi also stated “Despite concerted efforts, our investigators – both government and private sector, have not been able to demonstrate how the outbreak strain ended up in the affected factory.”
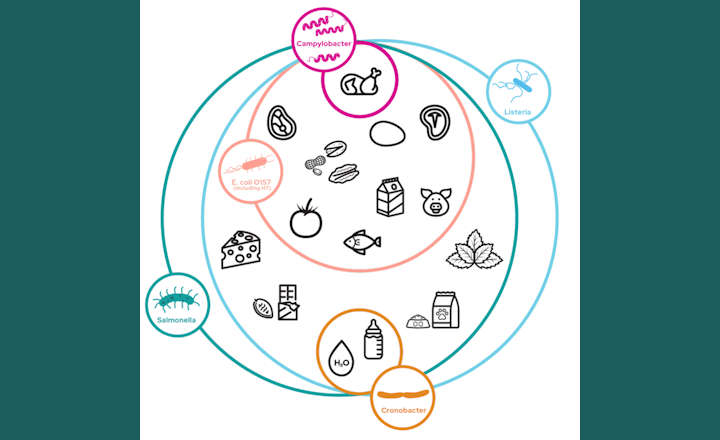
Lessons learnedL. monocytogenes occurs widely in agricultural, aquacultural and food processing environments, with higher prevalence in soils with higher moisture (Buchanan et al, 2017). The bacterium has been isolated consistently worldwide from raw and ready-to-eat meats, poultry, seafood, dairy products and vegetables (International Commission on Microbiological Specifications for Food, 1994). While control measures have reduced prevalence of L. monocytogenes across several food categories the rate of listeriosis has remained constant over the last decade (Buchanan op. cit.). Another notable outbreak occurred in Canada in 2008 linked to cold cut meats with 57 confirmed cases and 22 deaths.
The recent outbreak was however the deadliest listeriosis outbreak on record worldwide and South Africa was unprepared for an event of this magnitude, reflecting weakness in their current food safety system. Control of listeriosis can be a challenge to due several intrinsic factors, for example, the bacterium continues to multiply at refrigeration temperatures and can be highly resistant to disinfecting agents due to biofilm formation. As a result, controlling the spread of listeria requires careful, proactive measures throughout the processing chain. Shortages of in-country technical experts, auditors and qualified laboratory personnel in South Africa coupled with outdated regulations may hinder effective control.
Dr Anelich, Food Safety Specialist and Founder of Anelich Consulting commented in March 2018 regarding the outbreak saying “The South African food control system is quite fragmented…as it stands it is not ideal and needs to be revisited completely.”
HACCP point system standards while mandatory in many countries across the world is not in South Africa. She also commented that there is no maximum permissible level for L. monocytogenes in food in South Africa.
Likewise, Director for Food Control at the Department of Health Penny Campbell commented that the delays experienced in confronting regulatory gaps is due to both a lack of resources and prioritisation. The absence of an authoritative regulatory system may cause companies to lower standards of food production leaving consumers at risk thus the establishment of a definitive Food Safety Authority could help to mitigate such widespread outbreaks in the future.
The WHO advises that countries should strengthen their national food safety and disease surveillance structures to prevent this type of event occurring in the future. They are advised to immediately list listeriosis as a notifiable disease and to make use of various resources the WHO has developed such as the WHO Factsheet on Listeriosis and WHO manual to strengthen surveillance of and response to foodborne diseases.
Food safety laws have been updated with all factories that produce ready-to-eat processed meats and chicken now required to have food safety management systems in place according to regulation R607 published on June 14th, 2018.
Over the course of the outbreak, almost 900 health inspectors in all districts were retrained in factory inspections, food safety systems and testing of factories for Listeria. A total of 157 factories in total were identified with listeria and over 12,000 tons of food recalled and destroyed.
Further reading:
A review of Listeria monocytogenes: An update on outbreaks, virulence, dose-response, ecology and risk assessments www.sciencedirect.com/science/article/pii/S0956713516306892